Featured Medical Equipment
In-Stock and Ready for Quick Shipping
-
Byron Lysonix 3000 Liposuction Unit
Features: • PSI-TEC III Aspirator • EZ Pump Infiltrator • Lysonix 3000 Learn More -
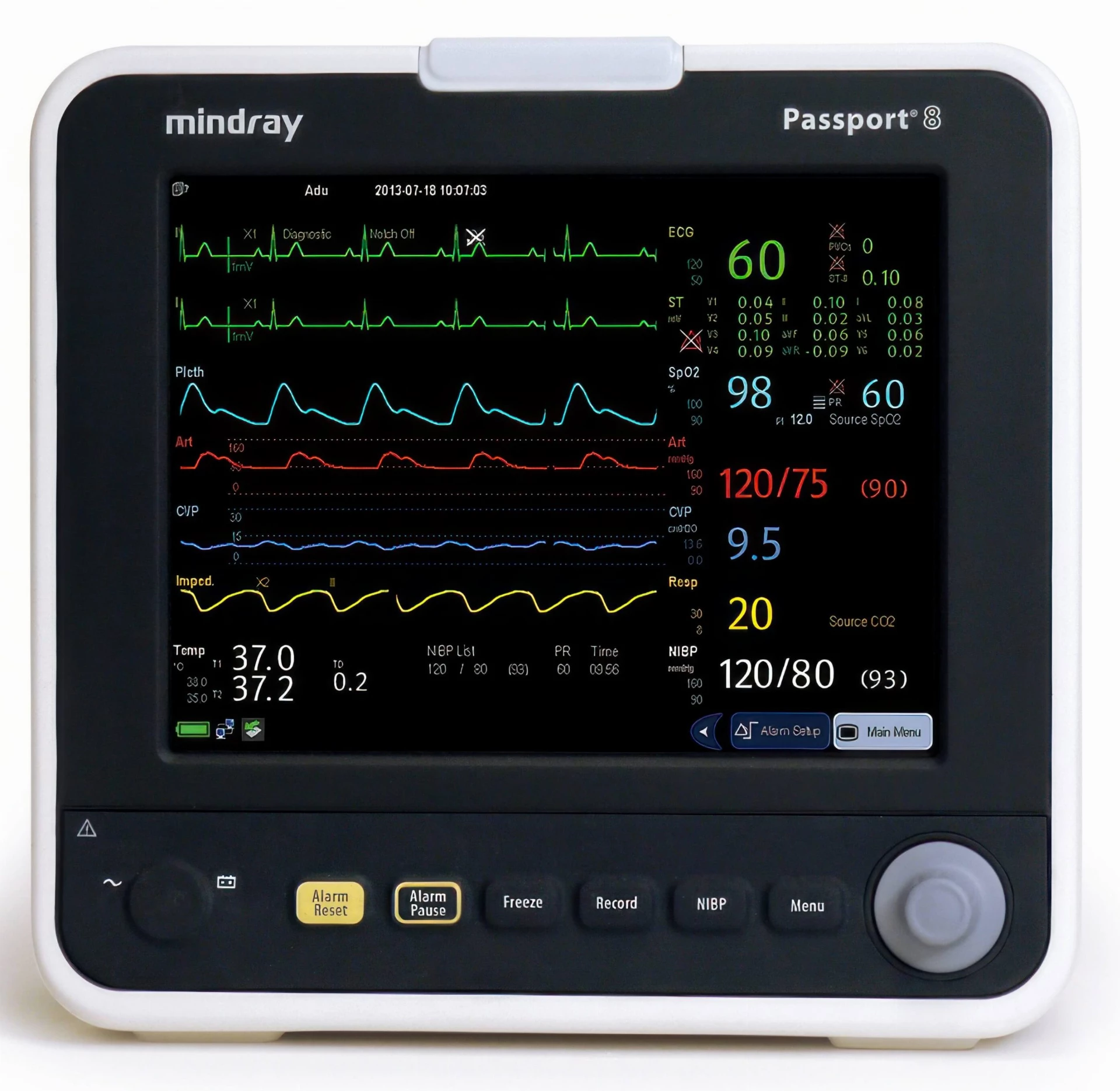
Mindray Passport 8 Patient Monitor
Mindray proudly offers the Passport 8, an inspired result of ingenuity and efficiency in the approach to the varying levels of patient ... Learn More -
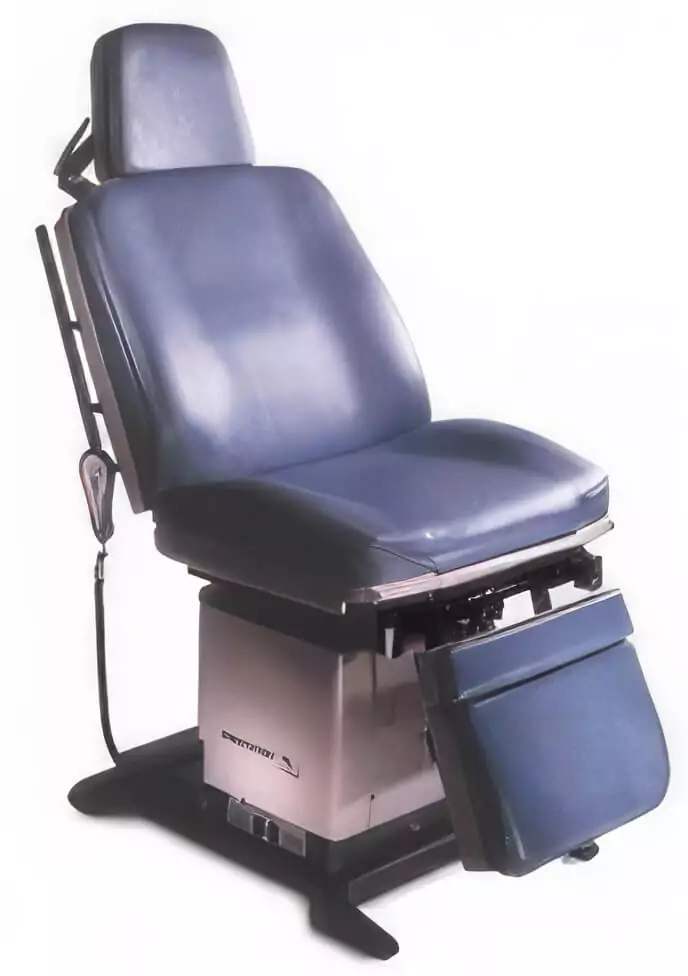
Midmark 230 Power Procedure Chair with Rotational Base
Includes Rotational Base, not removable. Extending the stirrups and treatment pan, lowering the foot support and tilting the seat ... Learn More -
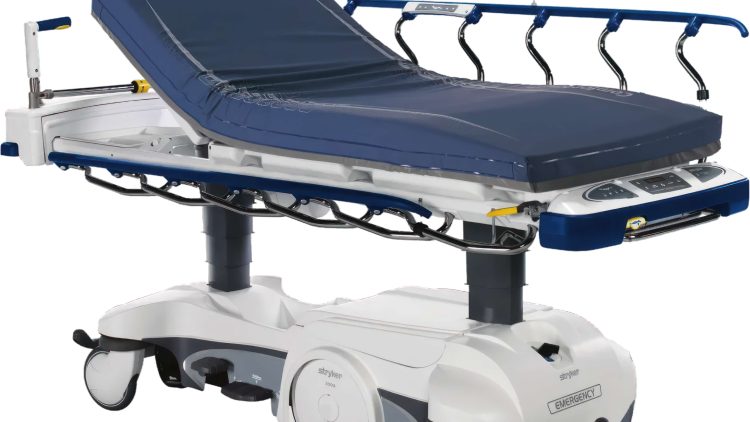
Midmark Ritter 75L
To help keep you and your staff fresh and alert all day, the Midmark® 75L does the heavy work. Full eight-way power, essential low ... Learn More
Repair and Maintenance Services
Biomedical Equipment
We provide a full line of Biomedical preventative maintenance, repairs, and calibrations onsite to keep you operating under NFPA99 standards and AAMI recommendations.
Sterilizers, Autoclaves, Washer Disinfectors, Boilers
Our Specialty is sterilization and keeping your facility operating under joint commission standards. We offer a variety of preventative maintenance programs that keeps your capital equipment running with little to zero down time.
Anesthesia Equipment
Auxo Medical provides services from inspection to comprehensive maintenance plans. We can structure a preventative maintenance agreement to meet you needs and budget. We are GE and Mindray certified.
Medical Equipment Bestsellers
-
Midmark Ritter M9 UltraClave (Autoclave), M9-022
The Midmark Ritter M9 Ultraclave automatic sterilizer is an autoclave that couldn’t be easier and is time tested for reliability. You ... Learn More -
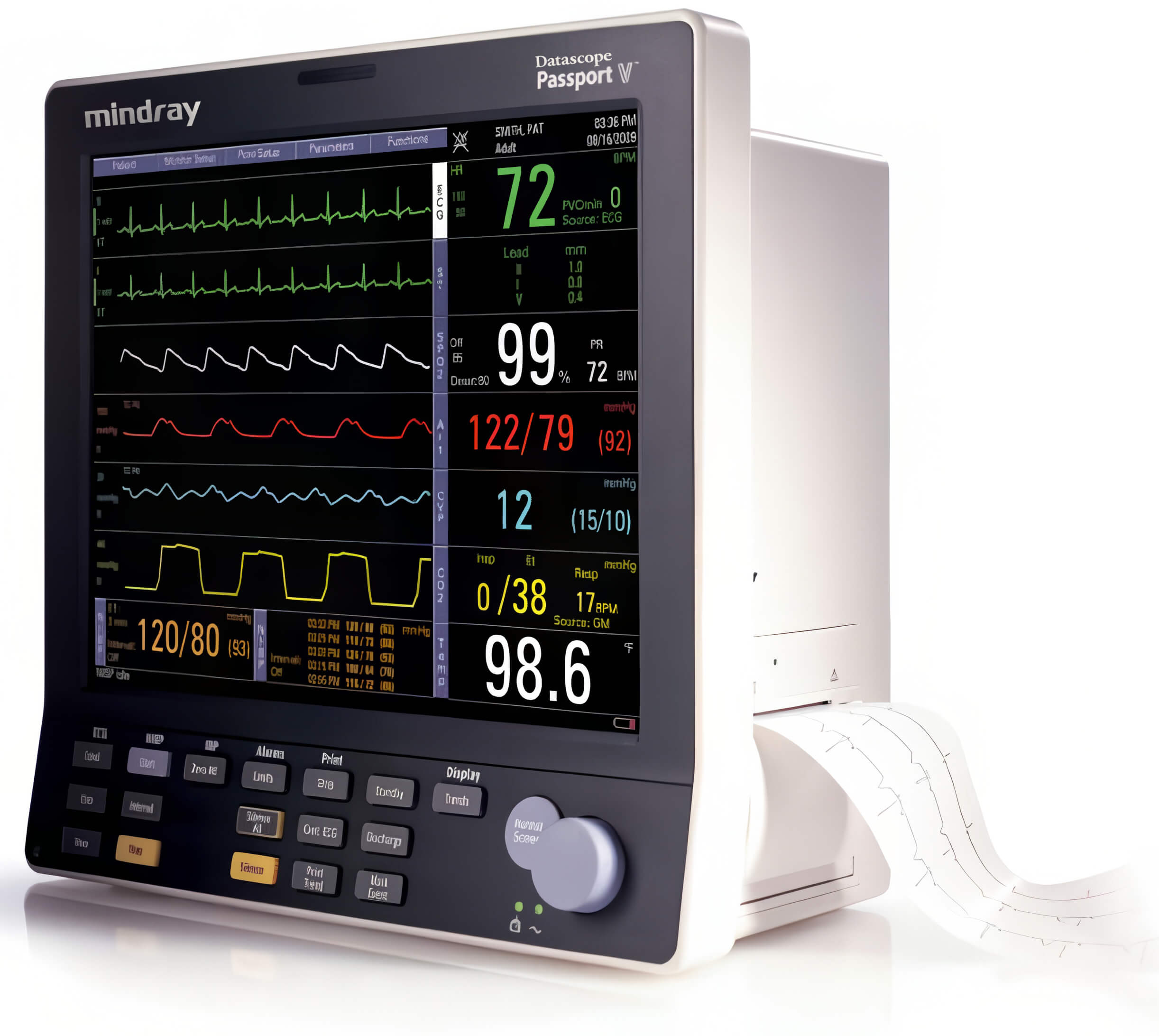
Mindray Datascope Passport V
The Passport V offers a comprehensive range of options that make it well-suited for most hospital departments. The flexible feature-set ... Learn More -
Steris Amsco Model 3085 Surgical Table
The Amsco 3085 General Surgical Table is one of the most reliable and popular surgical tables. Recognized as the industry standard due ... Learn More -
Steris V120 Steam Sterilizer
Steris Amsco Century Small Series, 20" x 20" x 38" Chamber, 250 Liters / 66 gallons The Century® Sterilizer meets the needs of ... Learn More
Additional Discounts and Trade-In
Get 5% discount off all equipment purchases.
Our sales associates can assess the “Market Value” of your facility’s medical equipment for trade-in or liquidation value. Liquidation services are primarily for facilities that are closing, merging, upgrading, or for insurance requirements.
Service Portal
The Auxo Medical Service Portal is a secure location where current service plan holders can manage their equipment inventory and track their support cases in real-time. Users can create new work orders submitted directly to the service team and also print repair and maintenance history reports on each of their assets. Need access to maintenance reports for your next survey or operational budget evaluation? All history is readily available in your Auxo Medical Service Portal.
Equipment Upgrades
Auxo Medical can also help you upgrade the equipment you currently have. We can upgrade or refurbish your current equipment onsite or remove and replace older equipment for a fraction of the cost of buying a brand new piece of equipment.
Testimonials & Reviews
I have had the pleasure to work with Anthony and the Auxo team over the last few months. Earlier this year, PartsSource utilized the services of Auxo for a new contract to include approximately 58 Steris sterilization devices. They were very thorough in communicating and completed PM inspections, repairs, and paperwork in a timely manner. The Auxo team went above and beyond to provide quality service at a significant cost savings in comparison to the OEM.
Auxo has become a preferred service provider for PartsSource and we will continue to work closely with them on future endeavors.
It has been a pleasure working and contracting with the Auxo Medical team over the last 15 years. As our businesses grew and evolved Auxo demonstrated they were willing to do what it took to support us both commercially as well as in services. These changes not only helped us optimize our overall business process flow it also allowed us to maximize our TCO’s on our equipment.
The Auxo Medical team is qualified to work on a vast array of equipment and systems. They’ve provided staff training, personalized service and attention to detail for the Past eight years.
The Auxo Medical team has been an outstanding partner. Their response to service calls has been stellar. We are very pleased with the management and tech support they provide.
Auxo Medical came into our facility a couple of months ago and has done an outstanding job by working with our staff and getting prior issues identified and resolved. They ran into many obstacles and worked diligently to remove them from our machines. Auxo has been a true partner with our organization.
I have used auxo to service my sterilization equipment for 15+ years at two separate facilities. They have knowledge of our facility, engineering staff, as well as our equipment. Auxo provides education to my staff on our sterilization equipment. You’ll be rewarded with great customer service. During a renovation project, auxo used a creative approach to keep us up and running during the entire process.
Working with Mark and Jay at Auxo for new client implementation has been nothing short of impressive. Some clients can be skeptical of switching their maintenance service from the OEM to third party service companies … however, after a brief meeting and walkthrough with the client and the team, it quickly becomes obvious. Auxo’s team members are truly industry experts. my clients rave about their responsiveness, expertise and focus to put the customer first. I can always count on them to go above and beyond for our clients … they are are pleasure to work with.
Mike Lunde is always very helpful and the communication is wonderful. Very thankful to have him on this team!
Wonderful customer service! Tanner has been so helpful in answering my many questions to make sure we purchase exactly what suits our needs. I would highly recommend Auxo Medical.
We had a problem with our anesthesia machine & called Auxo. Claude came out within 2 hours of our call and repaired it the same day. Excellent service! Highly recommend them!
Auxo Medical is a diamond in the rough and they deserve your business. Every aspect of my experience was top notch. I worked directly with Stark to set up my account. He was attentive, knowledgeable and very easy to work with. I Scheduled 2 maintenance visits for separate locations with Brandon and he absolutely delivered. My entire staff said he was great to be around and he left our lab cleaner than it was before. I definitely recommend Auxo Medical for anyone in need.
I have been managing surgery centers for several years and have always used AuxoMedical to perform preventative maintenance and repairs on our sterilization equipment. They are responsive, knowledgeable and reasonably priced. I have especially enjoyed working with Mark, Tanner and Tony. Highly recommended!
Mr. Claude McGuire is a phenomenal technician that has always been accommodating, professional and expedient in his work of keeping our autoclaves online and good to go! I would recommend Auxo Medical and their maintenance contracts - hopefully you'll get as lucky as we are to have Mr. McGuire service our sites.
Auxo's scheduled maintenance program has reduced our downtime by at least two thirds [and] response to problems has been lightning fast and repairs performed the same day in most cases. Auxo's overall performance has been outstanding. Previous agreements with other contractors were poorly performed resulting in chronic breakdowns and longer downtimes.
The Auxo Medical team has been amazing, by keeping some of our older equipment running as well as a new piece of equipment. They have also helped us update larger capital purchases for our surgery center. If you want reliable and fast service you couldn’t find a better team.