Featured Biomedical Equipment at Auxo Medical
At Auxo Medical, we specialize in providing high-quality, refurbished biomedical equipment that combines affordability with cutting-edge technology. Our curated selection ensures healthcare facilities can access reliable tools for diagnostics, surgery, and patient care without exceeding budgets. Below, we highlight five standout devices from our inventory, each rigorously tested and restored to meet OEM standards.
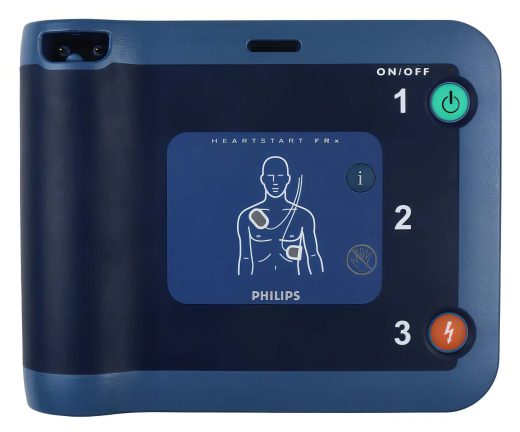
1. Philips HeartStart FRX AED with Wall Mount Box
A must-have for emergency preparedness, the Philips HeartStart FRX AED ensures rapid response during cardiac emergencies.
- Key Features:
- Infant/Child Key: Use adult pads on pediatric patients (unique to this model).
- Durability: Rugged, lightweight design with IP55 dust/water resistance.
- Wall Mount Included: Promotes visible, accessible storage.
- 1-Year Warranty: Backed by Philips’ reliability.
- Applications: Schools, gyms, offices, and public venues.
- Condition: Refurbished, with new battery, pads, and accessories.
2. GE MAC 5500 HD ECG System
Elevate cardiac diagnostics with the GE MAC 5500 HD ECG, renowned for precision and efficiency.
- Key Features:
- Advanced Algorithms: Detects Acute Coronary Syndrome (ACS) and paced rhythms.
- Barcode Workflow: Integrates with hospital systems for error-free patient data.
- 10.4″ Display: Full-page printouts and clear 12-lead reports.
- Applications: Hospitals, clinics, and cardiology departments.
- Condition: Refurbished, includes leadwires, electrodes, and operator manual.
3. Allen Yellofin Lift Assist Stirrups
Enhance surgical positioning with the Allen Yellofin Stirrups, designed for versatility and patient safety.
- Key Features:
- Pneumatic Lift Assist: Effortlessly adjust leg positioning mid-surgery.
- Squeeze Grip Handle: Sterile-field adjustments without contamination risks.
- 350 lb Capacity: Supports diverse patient sizes.
- Applications: Orthopedic, gynecologic, and urologic surgeries.
- Included: Legholders, bootpads, and table clamps.
4. Medfusion 3500 V6 Syringe Pump
Deliver precise medication with the Medfusion 3500 V6, featuring advanced safety protocols.
- Key Features:
- PharmGuard Integration: Reduces dosing errors with drug library support.
- FlowSentry™ Technology: Detects occlusions in real time.
- 10-Hour Battery: Ideal for transport or power outages.
- Applications: ICUs, oncology units, and pediatric care.
- Condition: Refurbished, with a bright LCD and horizontal syringe loading.
5. Valleylab Force FX Electrosurgical Unit (ESU)
Achieve precision in surgery with the Valleylab Force FX, a leader in electrosurgical innovation.
- Key Features:
- Instant Response™ Technology: Adjusts power automatically for consistent cuts and coagulation.
- Multiple Modes: Three cut, four coag, and three bipolar settings.
- Lightweight Design: <18 lbs for easy mobility.
- Applications: General surgery, laparoscopy, and ENT procedures.
- Condition: Refurbished, with reduced capacitive coupling risks.
Why Choose Auxo Medical?
- Comprehensive Refurbishment and Quality Assurance: All devices undergo inspection, rebuild and refurbishment, calibration, and testing.
- Cost Savings: Save 30–50% vs. new equipment.
- Warranty & Support: 1-year warranty, with maintenance and repair services available.
- Sustainability: Reduce e-waste with refurbished solutions.
Industries We Serve
- Hospitals & Surgery Centers
- Emergency Care & Clinics
- Long-Term Care Facilities
- Outpatient Surgery Units
Order your Biomedical Equipment from Auxo Medical
From AEDs to x-ray machines, Auxo Medical is your premier supplier of new and refurbished medical and lab equipment with nearly 1500 products available in our online equipment catalog. In addition view and request a quote or purchase directly from the featured biomedical equipment below:
-
Valleylab Force FX
The Valleylab Force FX™ generator offers surgeons precise power delivery, even through resistant tissue, thanks to its innovative Instant Response™ technology. This technology optimizes performance at lower power settings, reducing the risk of tissue damage, neuromuscular stimulation, and the need… -
Allen Yellofin Lift-Assist Stirrups (OEM# O-YFASI)
The Allen Yellofin Lift-Assist Stirrups (Hill-Rom/Allen OEM#: O-YFASI) are designed to enhance patient safety and ease of use during a variety of surgical procedures, including GYN, urological, laparoscopic, robotic, and colorectal procedures. These stirrups utilize patented Lift-Assist™ technology to neutralize… -
Philips Heartstart FRX AED w/ Wall Mount Box
The Philips HeartStart FRx AED is a state-of-the-art defibrillator, notable for its durability and user-friendly design. Backed by a 1-year manufacturer's warranty, this model uniquely offers an optional infant/child key, enabling the use of adult pads on pediatric patients. Lightweight… -
Medfusion 3500 V6 Syringe Pump
$2,195.00 The Medfusion 3500 V6 Syringe Pump, enhanced by PharmGuard Medication Safety Software, offers an intuitive and safe medication delivery system. Its large screen displays up to 30 characters per drug name, minimizing abbreviation errors, and the bright LCD backlight ensures…










 With increased employee turnover rates, compromised patient care, and elevated rates of errors, healthcare organizations are driving strategies to boost the well-being of their medical staff — including physicians, nurses, and support staff.
With increased employee turnover rates, compromised patient care, and elevated rates of errors, healthcare organizations are driving strategies to boost the well-being of their medical staff — including physicians, nurses, and support staff. Virtual Reality (VR) technology is paving the future for people, and patients, in more ways than you may realize. Here are five examples of how VR is enhancing the healthcare landscape.
Virtual Reality (VR) technology is paving the future for people, and patients, in more ways than you may realize. Here are five examples of how VR is enhancing the healthcare landscape.
