C-Arms for Sale: New & Refurbished Mobile Fluoroscopy Systems at Auxo Medical
Whether you’re outfitting a busy operating room, an ambulatory surgery center, or a specialty clinic, finding the right C-arm can make all the difference in procedural efficiency, image quality, and patient outcomes. At Auxo Medical, we carry over 30 high-quality C-arms from trusted brands like OEC, Genoray, Siemens, Hologic, and Fujifilm—available new, refurbished, and reconditioned to fit every budget and clinical need.
In this guide, we’ll walk you through what a C-arm is, why it matters, which models we currently offer, and how to choose the right mobile fluoroscopy system for your facility.
What Is a C-Arm?
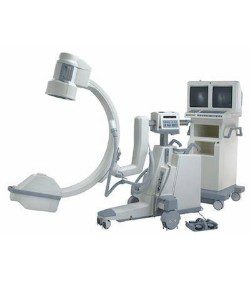
A C-arm is a mobile imaging device named for its distinctive C-shaped arm that connects an X-ray source on one end to an X-ray detector on the other. This unique architecture allows the device to rotate freely around the patient, delivering high-resolution, real-time fluoroscopic images without requiring patient repositioning.
C-arms are indispensable across a wide range of medical specialties, including:
- Orthopedics – Pinning fractures, verifying hardware placement, and checking bone alignment
- Pain Management – Guiding needle placement for epidural steroid injections and nerve blocks
- Vascular Surgery – Visualizing blood flow, identifying blockages, and guiding catheter-based interventions
- Cardiac Studies – Monitoring heart function during catheterization procedures
- Spine Surgery – Confirming pedicle screw placement and disc-level verification
- General Surgery & ERCP – Real-time guidance for minimally invasive procedures
Why Buy a C-Arm from Auxo Medical?
At Auxo Medical, we’re more than an equipment vendor—we’re your long-term imaging partner. Here’s what sets us apart:
- Extensive Selection – Our catalog features new and refurbished C-arms across multiple brands, detector types, and price points.
- Expert Guidance – Our team helps you match the right system to your procedural volume, specialty mix, and facility footprint.
- Maintenance & Repair Services – We offer proactive maintenance programs and expert repair to keep your C-arm performing at its best, minimizing downtime and extending equipment life.
- Quality Assurance – Every refurbished unit undergoes rigorous inspection, reconditioning, and testing before delivery.
- Affordability – Refurbished C-arms deliver exceptional imaging performance at a fraction of the cost of new systems, making advanced fluoroscopy accessible to facilities of all sizes.
C-Arm Models Currently Available at Auxo Medical
Below is a selection of the C-arm systems you’ll find in our C-arm product catalog. We regularly update our inventory, so contact us for the latest availability.
OEC C-Arms
The OEC brand (now part of GE Healthcare) remains one of the most recognized and trusted names in mobile fluoroscopy. We carry multiple OEC configurations:
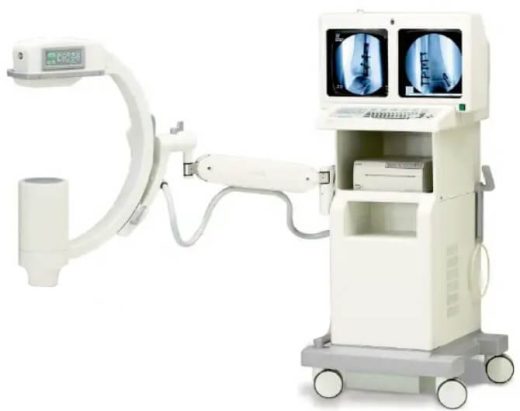
OEC 9800 C-Arm 12″ II General Surgery Package A proven workhorse for general surgical applications, the OEC 9800 with a 12-inch image intensifier provides reliable real-time imaging in a compact, maneuverable platform. Ideal for orthopedic, pain management, and general surgical procedures.
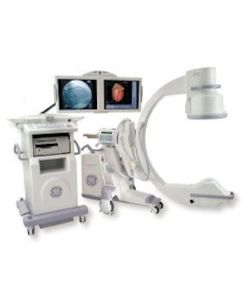
OEC 9800 with Super C-Arm and Dual High-Res 16″ Monitors For facilities requiring extended reach and a larger field of view, this Super C-arm configuration pairs the trusted OEC 9800 platform with dual high-resolution 16-inch monitors for enhanced visualization during complex cases.
Fujifilm Persona Series C-Arms (New)
We’re proud to offer five new Fujifilm Persona-series C-arms featuring advanced flat panel digital detector technology, exceptional image quality, and intuitive workflow design.
Fuji Persona C Compact C-Arm with 30cm Cesium Flat Panel Digital Detector
| Feature | Specification |
|---|---|
| Detector Size | 30 × 30 cm |
| Generator Power | 20 kW |
| Monitors | Dual 21.5″ touch monitors |
| Frame Rate | 25 FPS |
| Key Features | Radiography mode, removable grid, DICOM connectivity |
| Best-Fit Use Cases | Orthopedic, spine/pain, vascular, cardiac, ERCP |
This system delivers versatile, high-quality imaging in a compact footprint, making it an excellent choice for multi-specialty surgery centers and hospitals.
Fuji Persona C HR C-Arm with 30cm Flat Panel Digital Detector
| Feature | Specification |
|---|---|
| Detector Size | 30 × 30 cm |
| Generator Power | 25 kW |
| Monitor | 32″ 4K touch monitor |
| Frame Rate | 30 FPS |
| Key Features | IGZO detector, active cooling, snapshot/radiography modes, DICOM |
| Best-Fit Use Cases | Complex vascular, orthopedic, spine |
The Persona C HR is designed for the most demanding procedural environments. Its 25 kW generator and advanced IGZO detector technology deliver superior image clarity for complex vascular, orthopedic, and spine procedures where detail matters most.
Fuji Persona C Compact C-Arm with 21cm Cesium Flat Panel Digital Detector
| Feature | Specification |
|---|---|
| Detector Size | 21 × 21 cm |
| Generator Power | 20 kW |
| Monitors | Dual 21.5″ touch monitors |
| Frame Rate | 25 FPS |
| Key Features | Radiography mode, removable grid, DICOM connectivity |
| Best-Fit Use Cases | Orthopedic, vascular, cardiac, neuro |
A smaller detector footprint makes this model ideal for extremity work, neurological procedures, and facilities where a more compact imaging field is preferred.
Fuji Persona CS Compact C-Arm with 30cm Cesium Flat Panel Digital Detector
| Feature | Specification |
|---|---|
| Detector Size | 30 cm class (294 × 294 mm useful area) |
| Generator Power | 5 kW |
| Monitor | Integrated 27″ 4MP multi-touch monitor |
| Frame Rate | Up to 30 FPS |
| Key Features | Optional vascular package, DICOM connectivity |
| Best-Fit Use Cases | Minimally invasive surgical procedures |
The Persona CS platform is engineered for streamlined minimally invasive workflows with an integrated high-resolution monitor and ultra-compact design.
Fuji Persona CS Compact C-Arm with 21cm Cesium Flat Panel Digital Detector
| Feature | Specification |
|---|---|
| Detector Size | 21 cm class (205 × 205 mm useful area) |
| Generator Power | 5 kW |
| Monitor | Integrated 27″ 4MP multi-touch monitor |
| Frame Rate | Up to 30 FPS |
| Key Features | Optional vascular package, DICOM connectivity |
| Best-Fit Use Cases | Minimally invasive surgery, orthopedic, vascular, general |
Compact and efficient, this 21cm Persona CS model is perfect for ASCs and clinics performing high-volume minimally invasive orthopedic and vascular procedures.
How to Choose the Right C-Arm for Your Facility
Selecting the ideal C-arm depends on several key factors:
1. Procedural Mix and Specialty
Different specialties demand different capabilities. Vascular and cardiac procedures typically require larger detectors, higher frame rates, and greater generator power for optimal vessel visualization. Orthopedic and pain management cases may be well-served by a standard image intensifier or smaller flat panel detector.
2. Image Intensifier vs. Flat Panel Detector
- Image Intensifier (II) systems like the OEC 9800 are cost-effective, proven platforms ideal for general surgery and orthopedics.
- Flat Panel Detector (FPD) systems like the Fujifilm Persona series offer superior image uniformity, lower dose potential, a more compact detector housing, and no geometric distortion—making them the gold standard for vascular, cardiac, and complex spine work.
3. Facility Size and Mobility Needs
Consider hallway widths, OR dimensions, and how frequently the C-arm will be moved between rooms. Compact models like the Persona CS are designed for tight spaces and quick repositioning.
4. Budget: New vs. Refurbished
A refurbished C-arm from a trusted provider like Auxo Medical delivers clinical-grade performance at significantly reduced cost. Our refurbished OEC systems, for example, undergo comprehensive reconditioning to ensure reliability and image quality comparable to new equipment.
5. Service and Support
A C-arm is a long-term investment. We offer ongoing preventive maintenance and responsive repair services to protect your investment and minimize costly downtime.
The Benefits of Buying a Refurbished C-Arm
For many facilities—especially ambulatory surgery centers, chiropractic practices, veterinary clinics, and smaller hospitals—a refurbished C-arm offers the best balance of performance and value:
- Cost savings of 40–60% compared to new equipment
- Proven reliability from established platforms with extensive service histories
- Faster availability with shorter lead times than new system orders
- Sustainability through extending the useful life of quality medical equipment
- Full service backing from our in-house biomedical engineering team
C-Arm Maintenance and Repair Services
Keeping your C-arm in peak operating condition is essential for image quality, regulatory compliance, and patient safety. At Auxo Medical, we provide:
- Preventive maintenance programs tailored to your usage patterns and manufacturer recommendations
- Emergency repair services to get you back up and running quickly
- Tube replacements and detector calibration
- Software updates and system optimization
- Compliance documentation for Joint Commission, state, and federal inspections
Proactive maintenance not only extends the life of your C-arm but also helps avoid unexpected failures during critical procedures.
Who We Serve
Our C-arm solutions are trusted by a diverse range of healthcare providers, including:
- Hospitals and health systems
- Ambulatory surgery centers (ASCs)
- Orthopedic and spine surgery practices
- Pain management clinics
- Vascular and cardiac catheterization labs
- Veterinary surgical practices
- Chiropractic and sports medicine clinics
- University and teaching hospitals
Browse Our Full C-Arm Catalog
Ready to explore your options? Visit our complete C-arm product category page to view all available systems, specifications, and pricing. Our inventory changes frequently as new units arrive and existing systems find homes, so we encourage you to reach out directly for real-time availability.
Contact Auxo Medical
Whether you’re ready to purchase, need help comparing models, or want to schedule a maintenance consultation, our team is here to help.
Call us today at (888) 728-8448 or fill out our contact form to get started.
At Auxo Medical, we’re committed to providing healthcare facilities with high-quality, reliable imaging solutions—backed by expert service and support you can count on for years to come.
-
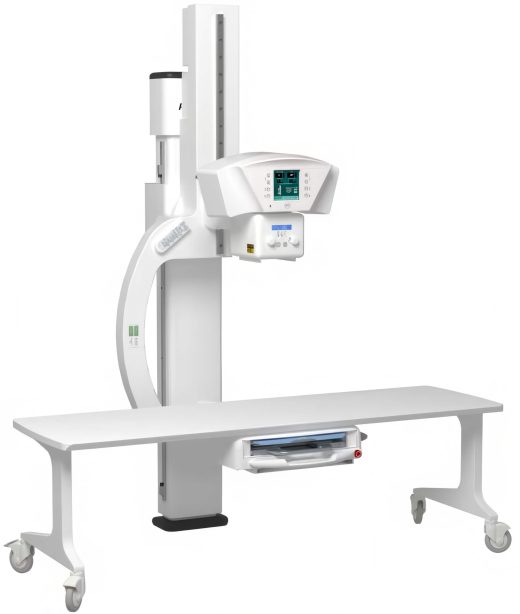
Fuji Digital Radiography U-arm System w/ 17×17 Detector and FDX Console Workstation
The Fuji Digital Radiography U-arm System with 17x17” detector and FDX Console Workstation offers a versatile, space-saving solution ideal for various clinical environments. Featuring the fully motorized Persona U, this single-detector DR system simplifies positioning with an innovative design that… -
Fuji Persona C Compact C-arm with 30cm Cesium Flat Panel Digital Detector
The Fuji Persona C Compact C-arm with 30cm Cesium Flat Panel Detector is an advanced, versatile imaging system optimized for fast, precise positioning in a wide range of diagnostic and minimally invasive procedures. Equipped with a high-resolution 30x30cm amorphous Silicon… -
Fuji Persona C HR C-arm with 30cm Flat Panel Digital Detector
The Fuji Persona C HR Mobile Fluoroscopy System with 30cm Flat Panel Digital Detector offers exceptional imaging capabilities tailored for complex vascular, orthopedic, and spine procedures. Combining high-power performance with a lightweight, maneuverable design, it features a robust 25 kW… -
Fuji Persona C Compact C-arm with 21cm Cesium Flat Panel Digital Detector
The Fuji Persona C Compact C-arm with 21cm Cesium Flat Panel Detector is an advanced fluoroscopy system designed for precise, high-quality imaging in minimally invasive procedures. Weighing approximately 280 kg (617 lbs) for the C-arm unit and featuring dual 21.5-inch… -
Fuji Persona CS Compact C-arm with 30cm Cesium Flat Panel Digital Detector
The Persona CS compact surgical C-arm is an advanced imaging platform designed for precise, high-quality visualization across a broad spectrum of minimally invasive procedures. Featuring a 30cm cesium iodide (CsI) flat panel detector, it offers multiple exposure modes—including ultra-low dose… -
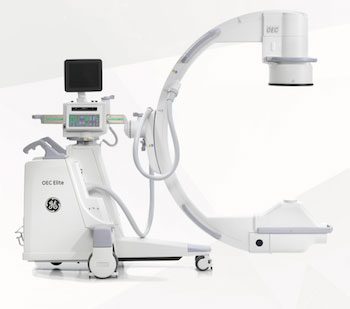
OEC GE OEC ELITE CFD 21cm Flat Detector C-Arm – General Surgery Package
Experience precision and clarity in every procedure with the GE OEC Elite CFD 21cm Flat Detector C-Arm General Surgery Package. Building on the trusted GE OEC 9900 lineage, this sixth-generation system replaces the traditional image intensifier with a 21 cm… -
OEC GE OEC ELITE CFD 31cm Flat Detector Super C-Arm – General Surgery Software Package
The GE OEC Elite CFD 31 cm Flat Detector Super C-Arm combines the trusted GE imaging heritage with a modern 31 cm CMOS Flat Panel Detector and a 32" UHD 4K monitor to deliver sharper, larger, and more accurate surgical… -
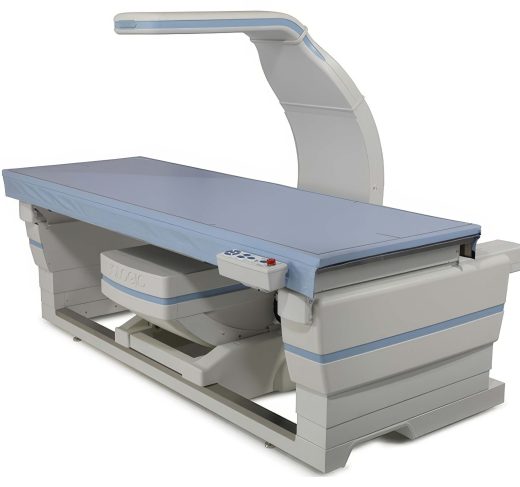
Hologic Horizon DXA System (W Model)
The Hologic Horizon DXA System (W Model) is a compact, high-performance bone density scanner designed for accurate, efficient measurements with minimal setup. Capable of supporting patients up to 500 lbs (227 kg), it features a 28-inch table height, 24-inch C-arm… -
MediCapture Medicap USB 200 Medical Image Recorder
$3,261.75 The MediCapture USB200 is the medical industry's easiest all-in-one digital video recording device, designed to seamlessly capture high-quality videos and still images directly onto any USB flash drive or optional hard drive—eliminating the hassle of DVDs. Compatible with ultrasounds, endoscopes,… -
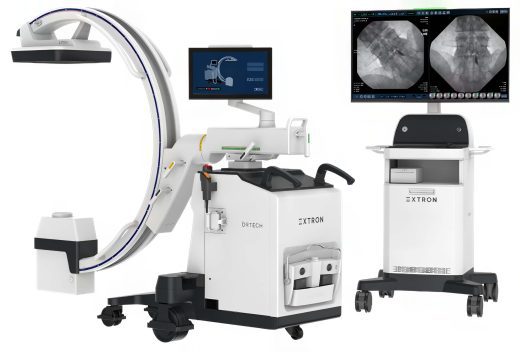
EXTRON 5 Premium C-Arm 30×30 Flat Detector
The DRTECH EXTRON 5 Premium C-Arm with a 30x30 flat detector is a high-end, low-dose imaging solution designed for demanding surgical environments. It combines a 30x30 dynamic flat-panel detector with a 43" 4K monitor, a versatile monitor cart, and advanced… -
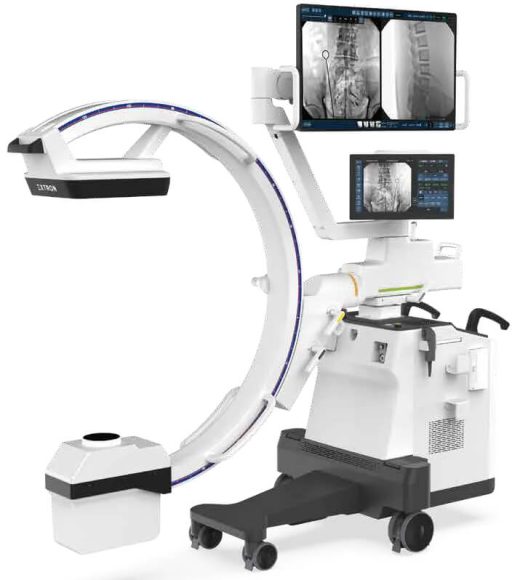
DRTECH EXTRON 5 Premium C-Arm 23×23 Flat Detector
DRTECH EXTRON 5 Premium C-Arm 23x23 Flat Detector is a top-tier, low-dose imaging system designed for demanding surgical environments where space and safety matter. It features a 23x23 dynamic flat-panel detector, a powerful 5 kW X-ray tube, and a 43"… -
MediCapture MediCap USB170 Medical Image Recorder
$3,261.75 The MediCapture MediCap USB170 is the medical industry’s most user-friendly and comprehensive image recording solution, designed to simplify the process of capturing and storing high-quality medical images. This rugged device records still images in standard definition directly from medical video… -
OEC 9800 C-Arm, 12” with Vascular Package & New Flat Panel Upgrade
The OEC 9800 C-Arm, 12” with Vascular Package & New Flat Panel Upgrade is a comprehensive imaging solution designed to enhance vascular and surgical procedures with advanced technology and versatile features. This system includes a dedicated Vascular Surgery Software Package,… -
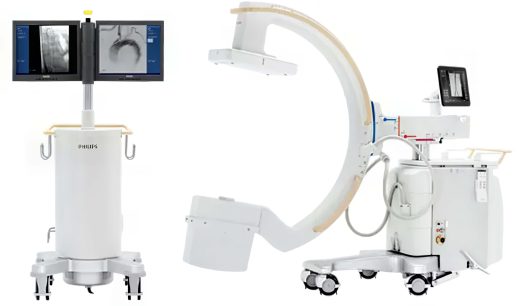
Philips Veradius Unity Flat Detector C-Arm
The Philips Veradius Unity Flat Detector C-Arm is a cutting-edge mobile imaging solution designed to enhance surgical precision and efficiency. Key features include a wireless foot switch, accurate repositioning with Position Memory, and Dose Aware real-time dose feedback, along with… -
OEC GE OEC ELITE CFD 31cm Flat Detector Super C-Arm – VAS 15 Software Vascular Package
The GE OEC Elite CFD 31cm Flat Detector Super C-Arm, equipped with VAS 15 Software and a Vascular Package, represents the pinnacle of mobile imaging advancements, evolving from the renowned GE OEC 9900. This sixth-generation GE OEC C-arm distinguishes itself… -
OEC GE OEC ELITE CFD 21cm Flat Detector C-Arm – VAS 15 Software Vascular Package
The GE OEC Elite CFD 21cm Flat Detector C-Arm with VAS 15 Software Vascular Package represents a significant upgrade in mobile imaging technology, building upon the legacy of the OEC 9900. This sixth-generation C-arm replaces the traditional image intensifier with… -
OEC 9900 Elite C-Arm, 12” with Vascular Package
The OEC 9900 Elite C-Arm with a 12” image intensifier and Vascular Package is a powerhouse imaging solution designed for precision and efficiency. Equipped with features like DICOM 3.0, a tri-mode image intensifier, and advanced 1kx1kx16 bit digital image processing… -
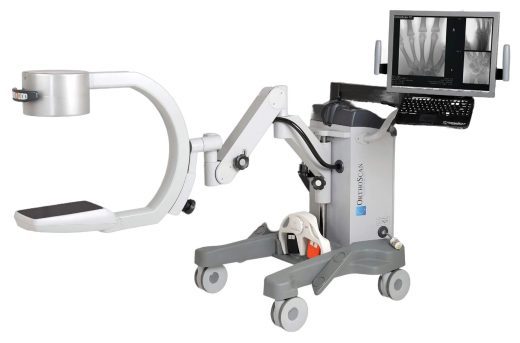
Orthoscan Pulse Mini C-Arm with Flat Detector
The OrthoScan Pulse Mini C-Arm with a Flat Detector represents a significant advancement in medical imaging technology, offering unparalleled precision and image quality. This cutting-edge device introduces pulsed fluoroscopy and boasts the largest flat detector in its class, ensuring exceptional… -
Orthoscan OR Mini C-Arm with Flat Detector
The OrthoScan FD mini c-arm with a flat detector and OR Version is a cutting-edge imaging solution designed to enhance surgical efficiency and patient comfort. Its innovative 150° orbital rotation and compact design facilitate optimal positioning within the surgical environment,… -
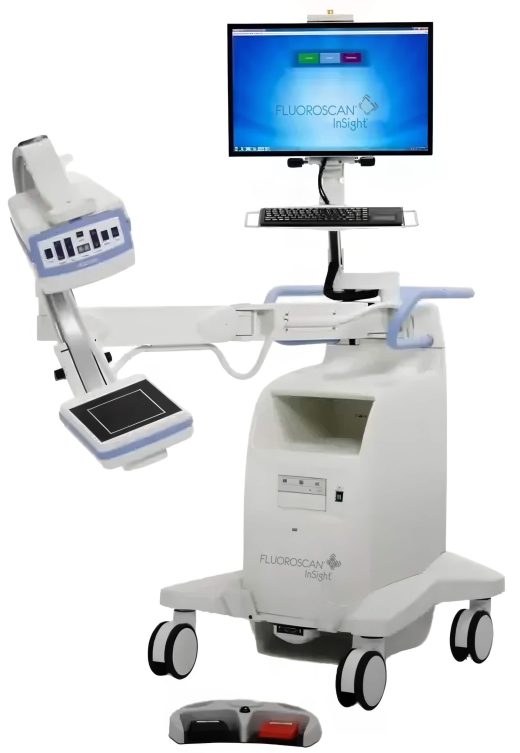
Hologic Floroscan InSight FD Mini C-arm
The Hologic Floroscan InSight FD Mini C-arm is a sophisticated imaging device designed to enhance surgical precision and ease of use. Featuring a dual field flat detector with a thin profile, this mini C-arm offers exceptional maneuverability, with a 90-degree rotation… -
MediCapture MVR PRO 409 (Medical Video Recorder)
The MediCapture MVR PRO 409 is a highly advanced medical recording device designed specifically to meet the demanding needs of modern operating rooms. It allows for effortless control either directly from its front panel or remotely via an external monitor… -
OEC 9900 C-Arm, 9” with Vascular Package
The OEC 9900 C-Arm with a 9” image intensifier and a specialized vascular package represents a pinnacle in advanced imaging technology designed for a wide array of interventional procedures. This precision-engineered equipment is tailored to meet the intricate needs of… -
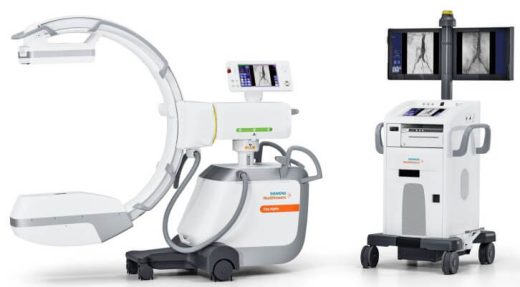
Siemens Cios Alpha C-arm with Vascular Package
Patient Ready Cios Alpha Cios Alpha is a high-end C-arm system with a dynamic flat detector for fluoroscopy and acquisition of single images. The compact, mobile system is designed for use in cardiovascular surgery, gastroenterology, urology, emergency surgery, orthopedics and… -
Fuji Persona CS Compact C-arm with 21cm Cesium Flat Panel Digital Detector
The Persona CS Compact Surgical C-arm, featuring a 21cm cesium iodide (CsI) flat panel detector, offers an advanced, versatile imaging solution optimized for fast, precise positioning and exceptional image quality across a wide range of minimally invasive surgeries. Designed with… -
Orthoscan Mini C-Arm Flat Detector
OrthoScan FD mini c-arm with a flat detector. This flat detector design and compact form factor allows optimal positioning in the surgical environment. Exceptional image quality by increased grayscale improves diagnostic accuracy. User-driven design allows optimal image quality with minimal… -
Hologic Insight II Mini C-arm
The Fluoroscan InSight 2 mini C-arm is an intuitive and easy-to-use, cost effective system designed specifically for the orthopedic and extremity imaging market. With high quality digital images, simplified operation and easy mobility, the system is the ideal choice for… -
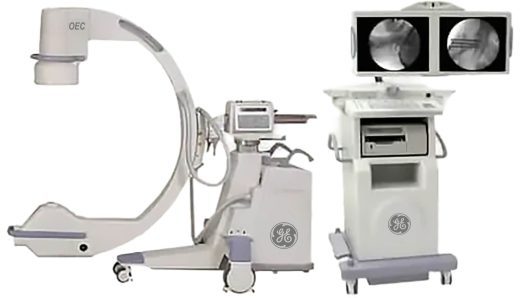
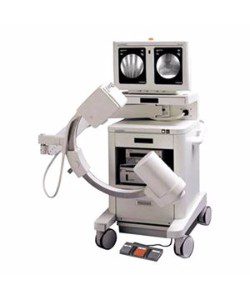
OEC 9800 C-arm 12″ ii General Surgery Package
The OEC 9800 is the gold standard in mobile fluoroscopy applications and innovative X-ray imaging technology. Built on the leadership and experience of thousands of systems installed world-wide, GE has set a new standard in mobile C-arm imaging with the… -
OEC 9800 with 9″ Image Intensifier and ESP Package
The OEC 9800 is the gold standard in mobile fluoroscopy applications and innovative X-ray imaging technology. Built on the leadership and experience of thousands of systems installed world-wide, GE has set a new standard in mobile C-arm imaging with the… -
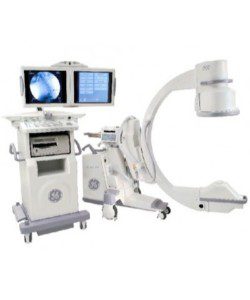
OEC 9800 with Super C-Arm and Dual High Res 16″ Monitors
The OEC 9800 is the gold standard in mobile fluoroscopy applications and innovative X-ray imaging technology. Built on the leadership and experience of thousands of systems installed world-wide, GE has set a new standard in mobile C-arm imaging with the… -
OEC 9800 C-Arm, 9″ Super C with GSP & Flat Panel Upgrade
The OEC 9800 is the gold standard in mobile fluoroscopy applications and innovative X-ray imaging technology. Built on the leadership and experience of thousands of systems installed world-wide, GE has set a new standard in mobile C-arm imaging with the… -
OEC 9600 C-Arms
The OEC 9600 Digital Mobile C-Arm provides great images with low dose exposure. The 9600 is maneuverable, is simple to operate, & provides large images. Originally manufactured between 1994-2000. [vc_btn title="Download Brochure" style="flat" shape="square" link="url:/wp-content/uploads/2017/06/OEC-9600-C-Arm-Auxo-Brochure.pdf ||target: _blank|" css=".vc_custom_1479498791367{margin-left: 5px !important;padding-right:…









































 Anesthesia systems are complex, safety-critical devices that demand disciplined maintenance. When anesthesia equipment is overdue for inspection or starts to drift out of specification, the risk is not only operational. It can affect patient safety and clinical confidence.
Anesthesia systems are complex, safety-critical devices that demand disciplined maintenance. When anesthesia equipment is overdue for inspection or starts to drift out of specification, the risk is not only operational. It can affect patient safety and clinical confidence.